
Research shows that between 40% and 80% of what patients are told during a healthcare consultation is forgotten immediately, and of what remains, almost half is remembered incorrectly*. For patients managing chronic conditions that's not just inconvenient – it's clinically significant, and potentially life threatening.
Using AI assisted transcription and summation we created a product that empowers patients to take better control of their care, improving adherence and patient outcomes.
*Source: https://pmc.ncbi.nlm.nih.gov/articles/PMC539473/

The challenge.
The gap between what a GP says to do and what a patient actually does next is well documented – and well ignored. The consultation ends, the patient leaves, and the instructions given verbally begin to fade almost immediately. The results of this are wholly predictable issues: missed medications, misunderstood dosing, forgotten referrals. The consequences compound quietly, over time, until they become harder –and more expensive – to address.
Drug non-adherence costs the NHS more than £500 million every year**. Even more troubling from a patient outcomes perspective us that up to half*** of all medicines prescribed for long-term conditions are not taken as recommended – not because patients don't want to follow their treatment plan, but because the system expects them to rely on memory alone.
Attempts at technological solutions hadn't kept pace with the problem: texted summaries were inconsistent, “patient portals” were underused and generally unliked. Follow-up calls placed an additional burden on healthcare services already stretched to their limit, and any other insertion into overstuffed GP workflows was a non-starter.
The result was a system that expected patients to retain, interpret and act on clinical advice in a context - the post-consultation journey home - where they are least equipped to do so.
**Source: https://pharmatimes.com/news/drug_non-adherence_costing_nhs_500m_a_year_1004468/
***Source: https://www.ncbi.nlm.nih.gov/books/NBK55438/

The approach.
We began by mapping the full consultation journey - from the moment a patient enters the room to the point at which they're expected to act on clinical advice at home.
Speaking directly with both clinicians and patients, we found that the problem wasn't memory alone, it was clarity, confidence and - perhaps most importantly of all - context. Patients often knew they'd been told something important, they just couldn't recall what it was, or what specifically they were supposed to do with it.
We worked closely with clinical and technical stakeholders to explore how voice-to-text technology could capture consultations passively, without disrupting the natural dynamic between GP and patient - then iterated on AI-generated summary formats based on real patient comprehension and recall testing.
The question throughout wasn't just "how do we transcribe this?" It was "what does a patient actually need to enable them to walk away and do the right thing?" and perhaps most importantly - “when is the best time to tell them?”

The solution.
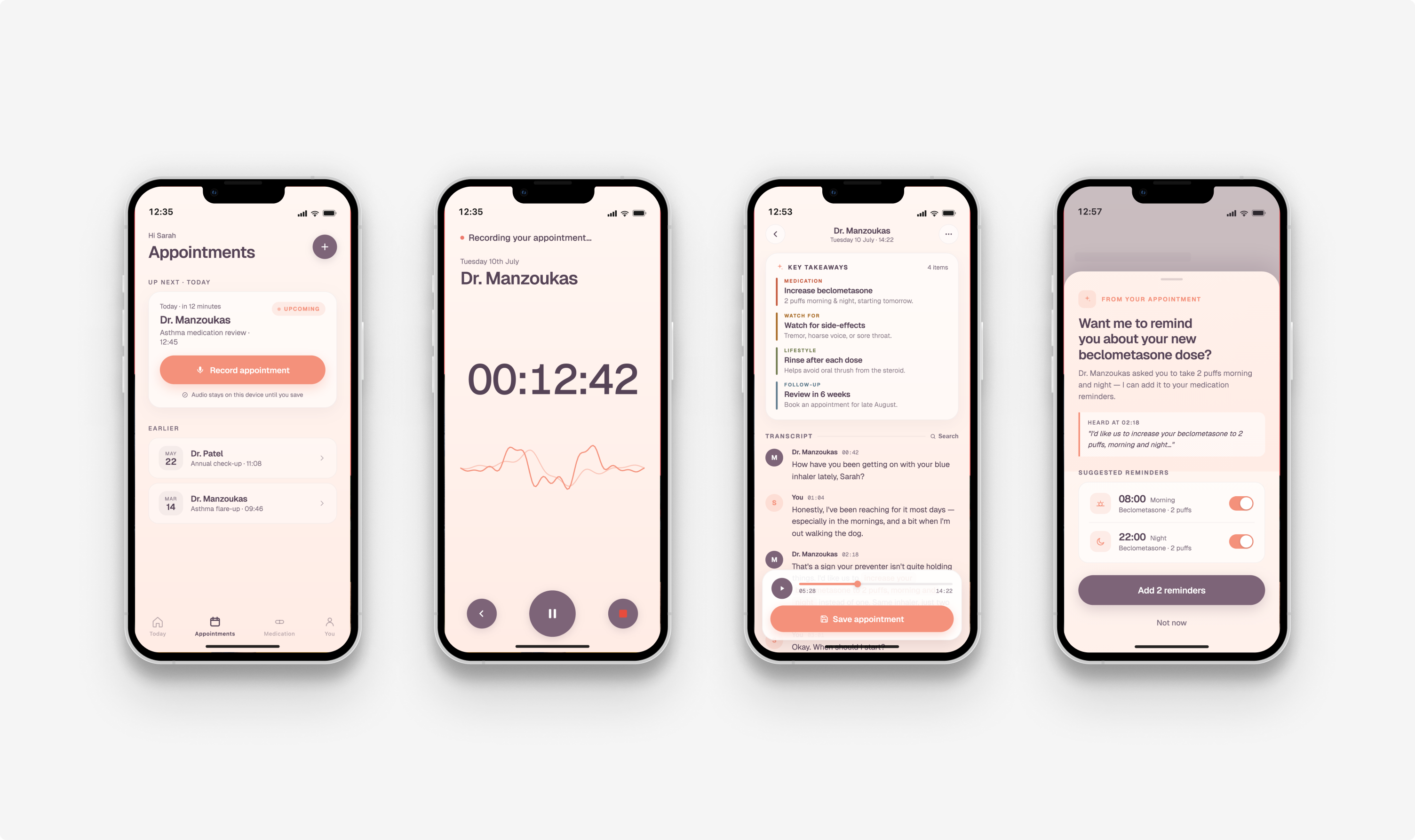
A streamlined workflow that automatically captures the GP consultation, extracts what matters, and delivers clear, personalised messaging. The system doesn't just summarise - it understands, using AI to identify what the patient needs to do, delivered in language they can act on, at the right time to act.
Key features of the solution:
- Passive voice capture - consultations recorded without disrupting the GP-patient dynamic
- AI-assisted messaging - clinically relevant content distilled into plain language, personalised to the patient
- Timely interventions - medication reminders, follow-up prompts and guidance scheduled to surface at the moment they're most likely to be acted on
- Designed for complexity - built specifically for patients managing multiple long-term conditions, where the risk of poor adherence is highest
The outcomes.
In our testing, patients reported feeling significantly more confident in managing their own care. Clinicians noticed a reduction in follow-up calls from confused patients, and an increase in patients arriving at subsequent appointments having acted on the advice they'd been given.
Adherence to prescribed treatment plans improved measurably across the patient cohort, with the greatest gains seen in patients managing multiple long-term conditions - historically the hardest group to support effectively.
The aggregated, anonymised consultation data also gave commissioners a richer picture of patient need across the practice network - enabling more targeted interventions and better resource planning.
The clinical advice was always there, the problem was getting it to stick.



