
*Source: National Diabetes Inpatient Audit, 2017 (via PMC6473239)
For the nurses and healthcare professionals (HCPs) responsible for managing patients on insulin pump therapy, programming a pump is one of the most consequential tasks in their working day. Yet the interfaces designed to support it have historically made the job harder than it needs to be - dense, slow and poorly suited to the pressures of a busy clinical environment.
PharmaSens developed their niia patch pump system to change what insulin therapy could feel like for patients. We worked with them to make sure the clinical experience for HCPs matched that ambition - designing an interface that surfaces the right information at the right moment, and makes the setup and management of treatment as straightforward as it should be.

The challenge.
Programming a patient's basal insulin regimen has traditionally meant navigating numeric tables: rows and columns of values requiring careful manual entry and cross-checking against patient lifestyle history. It's slow, cognitively demanding, and in a busy clinical environment where a nurse may be managing multiple patients in a session, it's a process where errors can happen.
Traditional on-device interfaces placed significant demands on nurses - fiddly to navigate, slow under time pressure and difficult to use when reviewing patient history at a glance. A tablet companion application offered the opportunity to change that entirely.
Our brief was to design an interface that made the process faster, clearer and more forgiving – one built around how nurses actually think and work, not how the back end software does.
The approach.
We spent time with diabetes nurses to understand the reality of their workflows – not just the steps involved in programming a pump, but the pressures around those steps. What emerged was consistent: the numbers-first approach of existing interfaces asked too much. Nurses were navigating dense data entry screens while simultaneously holding clinical decisions in their heads. The stress this created wasn't just unpleasant – it was a risk factor.
That insight shaped everything that followed. We ran an iterative, human-centred design process, moving through concept, prototype and usability testing in close collaboration with nurses at each stage. Nothing was finalised until it had been validated with the people using it.
We also worked closely with the development team throughout, ensuring the embedded application was designed and documented to meet regulatory submission standards - including formal Human Factors studies to evidence the system's safety and usability.

The solution.
The application replaced the complexity of traditional pump programming with a clear, graphical interface built around three core capabilities:
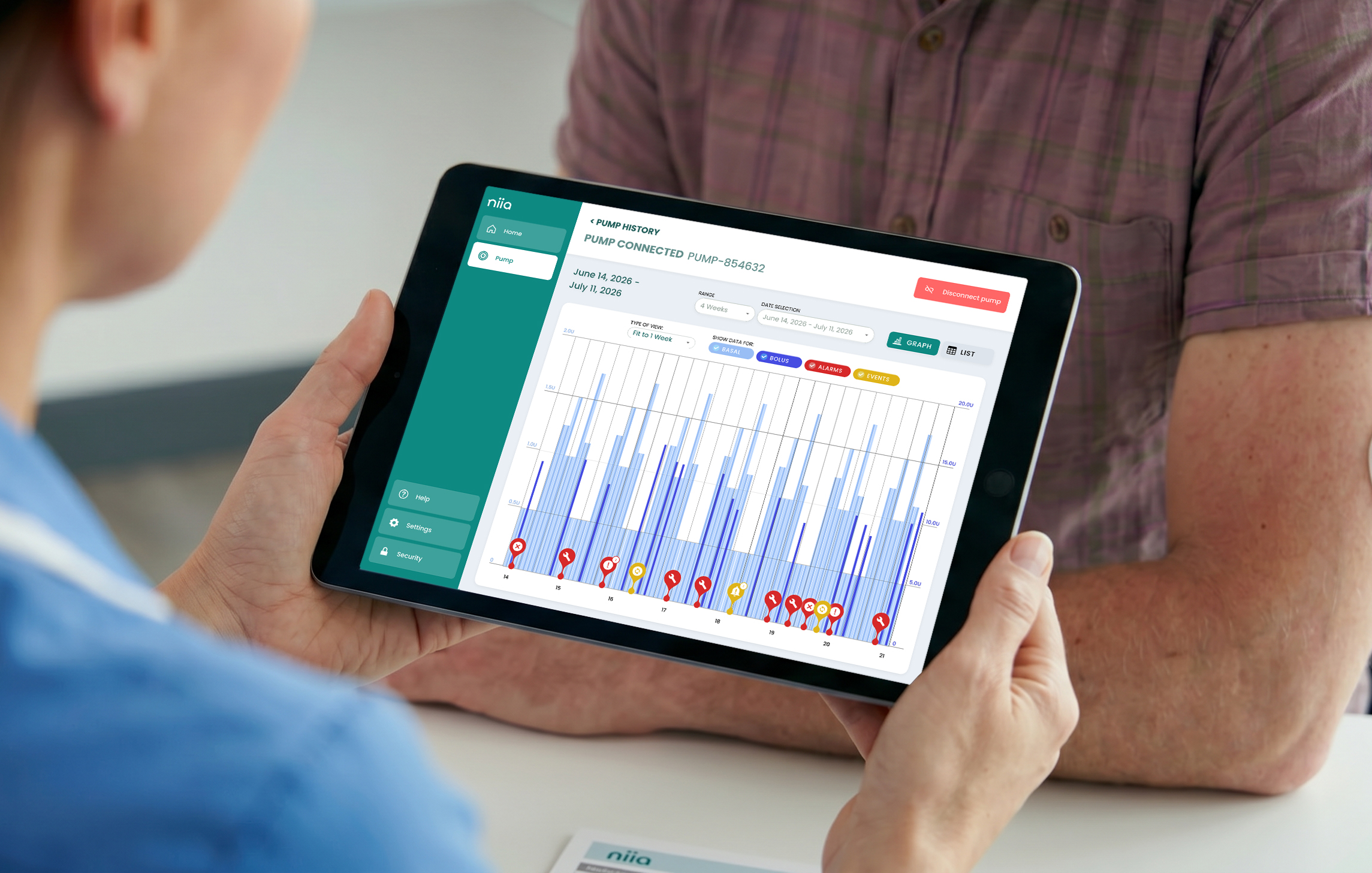
- Graphical basal profile setup - the patient's insulin regimen is presented as a visual timeline rather than a numeric table, making it faster to configure and easier to adjust with confidence
- Treatment history visualisation - key events and readings are surfaced in a structured, chronological view, giving nurses the context they need to make treatment decisions without digging through raw data
- Future ready interface - to support PharmaSens’ vision to produce a fully integrated patch pump, incorporating both insulin delivery and constant glucose monitoring, the interface allows room for future expansion and an additional layer of information
We also produced regulatory-grade documentation to support the project through approval. Human Factors studies were conducted throughout, with detailed documentation produced at each stage to support the regulatory pathway and give PharmaSens confidence in the evidence base behind the design.
The outcomes.
Every nurse who participated in the validation study - 100 diabetes nurses based in the USA - indicated they would recommend the device over others currently on the market.
That result reflects something broader than interface preference. Nurses described the graphical approach as genuinely more intuitive than anything they had used before - not a marginal improvement, but a meaningfully different experience of the same task. Setting a basal profile became faster. Reviewing patient history became clearer. The cognitive load of the programming process - and the stress nurses had consistently described as part of their day - decreased.
For patients, a more confident, less pressured clinical team means lower risk of errors in the setup and management of their treatment. For PharmaSens, the project delivered a validated, regulatory-compliant application with the documented evidence to support market entry - and a clinical interface that strengthens the case for their device among the nurses whose confidence in it matters most.



